 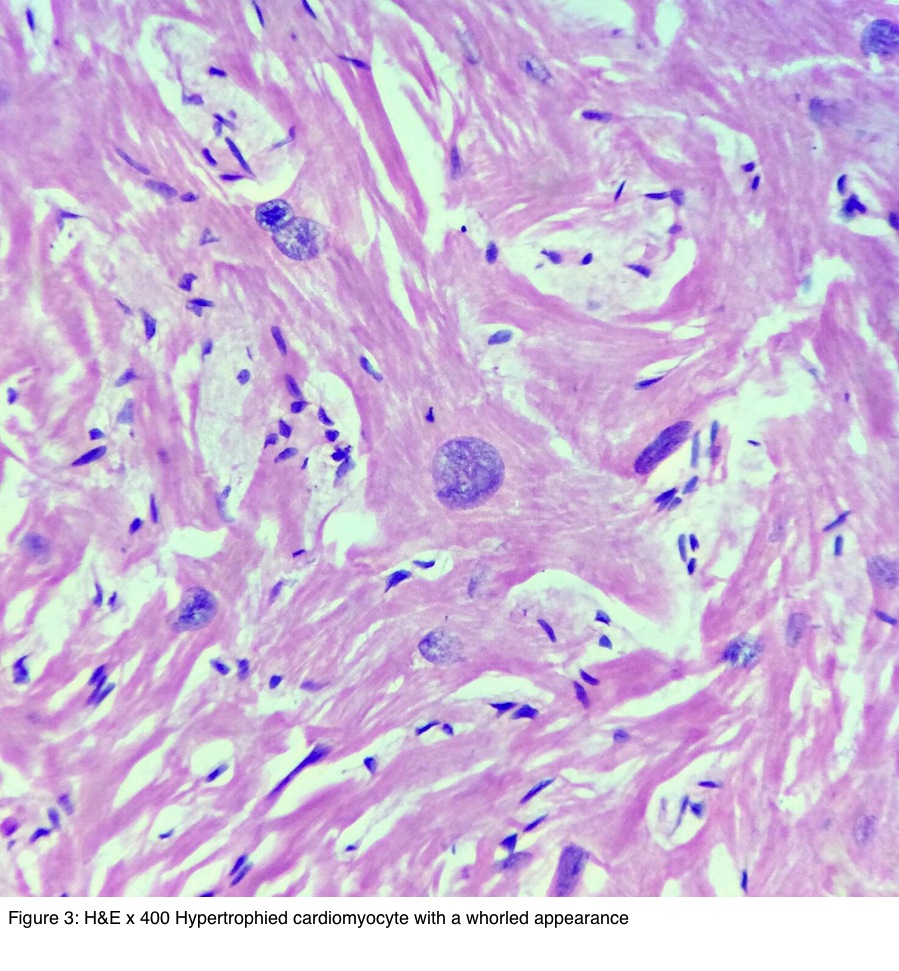
Pathologic hypertrophy occurs due to volume and/or pressure overload, storage and infiltrative disease, systemic disorders, and cardiomyopathies. It is defined as a balanced type of eccentric hypertrophy. Physiologic hypertrophy is typically observed in people undergoing regular strenuous dynamic exercise (“athlete’s heart”) and during pregnancy. This will allow to perform clinic-pathological correlation and to detect genetically determined forms. The goal of our paper is therefore to provide a uniform terminology and methodology to assess cardiac hypertrophy at gross and histologic examination of the heart, and also reference values available covering the range of “normal” cardiac measurements. Finally, in some cases, the cause of hypertrophy remains unexplained after in-depth gross and histologic examination, and it should then be designated idiopathic left ventricular hypertrophy (LVH). This approach allows us to address the genetic form of hypertrophic cardiomyopathy (HCM) which is currently considered as “primary” cardiomyopathy, where the major distinctive feature is histological disarray of myocytes. However, in order to reach a final diagnosis, systematic histologic analysis is mandatory, integrated with special stains, immunostaining, and transmission electron microscopy (TEM) when appropriate. A number of gross morphologic features can indeed point to a specific diagnosis, such as concentric hypertrophy, biventricular hypertrophy, outflow tract obstruction, thickening of the interatrial septum, nodular thickening with calcification of the aortic valve, systemic and other organ involvement, and obesity. The diagnostic work-up in the setting of cardiac hypertrophy implies delineation of disease entities with hypertrophic hearts including pressure and volume overload conditions, compensatory hypertrophy, storage and infiltrative disorders, and cardiomyopathies. Interpretation of these findings needs a proper knowledge of the pathologic backgrounds of hypertrophy, including “new” diseases and adherence to the current insights obtained from clinical imaging (echocardiography, computed tomography-CT, cardiac magnetic resonance-CMR). 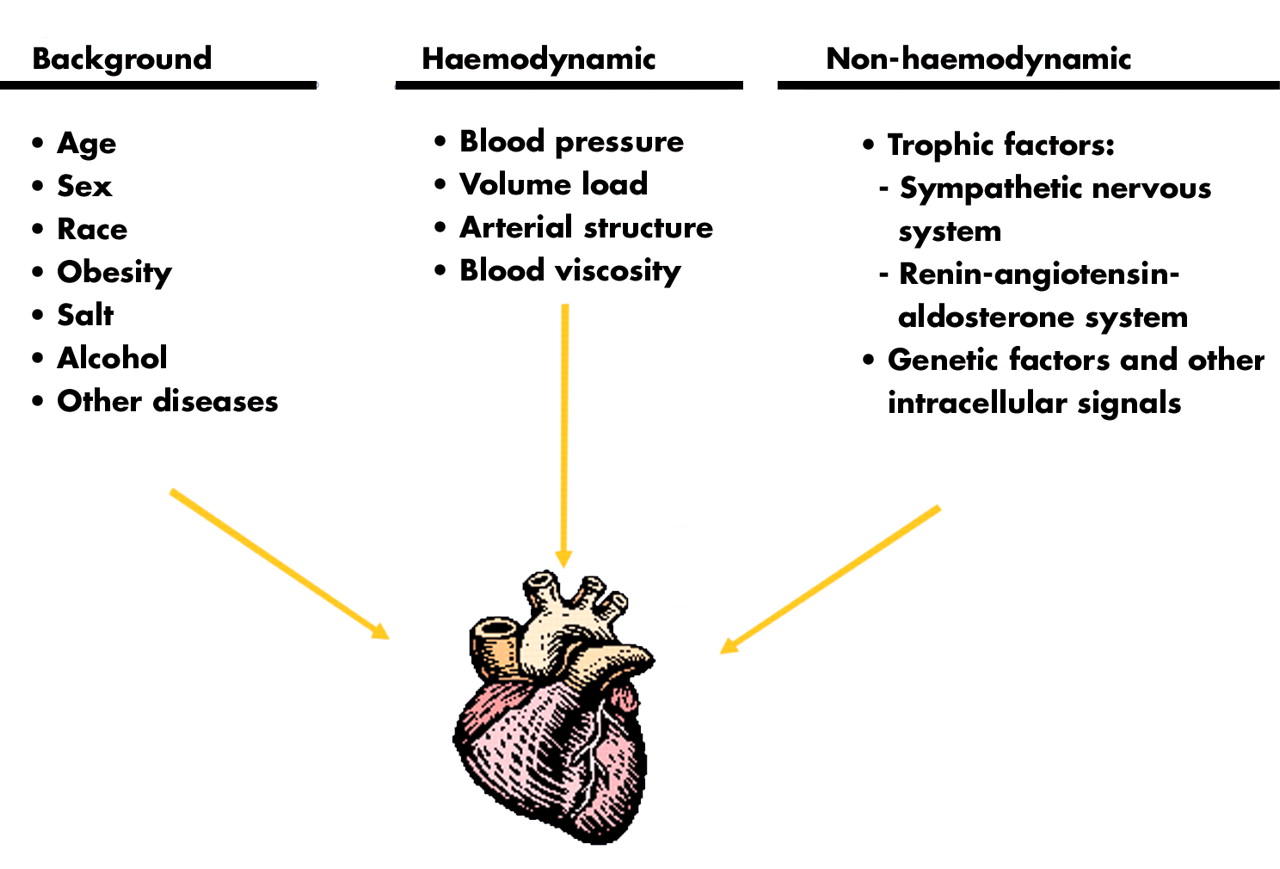
Assessment of the cardiac dimensions at autopsy requires a uniform approach, including terminology, a common methodology to measure the heart weight, size, and thickness as well as a systematic use of cut off values for normality. Why is there a need for a document on the pathologic diagnosis of cardiac hypertrophy? This is a very important issue as cardiac hypertrophy could be considered as a cause of death. In clinical autopsies, especially those with complex multiorgan disease, the contribution of heart failure (either left or right sided, or both) to the death of a patient is frequently a matter of discussion. For example, in case of sudden death, when the only finding is increased cardiac mass, the pathologist should search for features which could suggest a possible genetic etiology and eventually advice the families for clinical and genetic counseling. The main challenge is to determine whether these features are physiological or pathological, and if they could represent the substrate for arrhythmogenesis or heart failure. The clinical and forensic pathologists are frequently faced with increased heart weight and heart size, with or without increased wall thickness or chamber dilatation at autopsy. Indication for postmortem genetic testing should be integrated into the multidisciplinary management of sudden cardiac death. If the autopsy is carried out in a general or forensic pathology service without expertise in cardiovascular pathology, the entire heart (or pictures) together with mapped histologic slides should be sent for a second opinion to a pathologist with such an expertise. Although some gross morphologic features can point to a specific diagnosis, systematic histologic analysis, followed by possible immunostaining and transmission electron microscopy, is essential for a final diagnosis. The diagnostic work up implies the search for pressure and volume overload conditions, compensatory hypertrophy, storage and infiltrative disorders, and cardiomyopathies. For these reasons, recommendations have been written on behalf of the Association for European Cardiovascular Pathology. Common terminology and methodology to measure the heart weight, size, and thickness as well as a systematic use of cut off values for normality by age, gender, and body weight and height are needed. Since cardiac hypertrophy may be considered a cause of death at autopsy, its assessment requires a uniform approach. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
